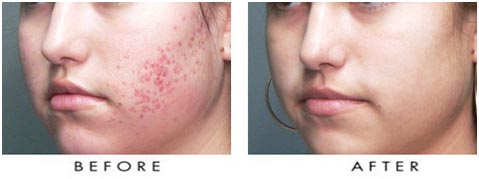
Acne Treatment in Punjabi Bagh By Dr. Vijay Singhal at Zenith Skin & Dental Clinic
Are you tired of dealing with acne and its aftermath? Do you dream of having clear, radiant skin that boosts your confidence? Look no further! Dr. Vijay Singhal at Zenith Skin & Dental Clinic in Punjabi Bagh is here to help. As a renowned dermatologist, Dr. Singhal provides expert acne treatment in Punjabi Bagh that addresses the root cause of your skin concerns.
Understanding Acne: What is it and Why Does it Happen?
Acne is a common skin condition that occurs when the pores on your skin become clogged with dead skin cells, oil, and bacteria. It can cause a range of symptoms, from mild blackheads and whiteheads to severe cysts and nodules. But why does it happen? The exact cause of acne is still unknown, but factors like hormonal fluctuations, genetics, and stress can contribute to its development.
Types of Acne: Whiteheads, Blackheads, and More
Did you know that there are different types of acne? From comedonal acne (whiteheads and blackheads) to inflammatory acne (papules, pustules, and cysts), each type requires a unique approach to treatment. Understanding your acne type is crucial for effective treatment.
The Importance of Professional Acne Treatment
While over-the-counter treatments may provide temporary relief, professional acne treatment is essential for long-term results. A dermatologist like Dr. Vijay Singhal can help you identify the underlying causes of your acne and create a personalized treatment plan.
Dr. Vijay Singhal: Your Go-To Dermatologist in Punjabi Bagh
With years of experience in dermatology, Dr. Vijay Singhal is the go-to expert for acne treatment in Punjabi Bagh. At Zenith Skin & Dental Clinic, he uses the latest technology and techniques to provide effective solutions for acne and other skin concerns.
Acne Treatment Options at Zenith Skin & Dental Clinic
At Zenith Skin & Dental Clinic, Dr. Singhal offers a range of acne treatment options, including:
- Chemical Peels: A non-invasive solution that exfoliates the skin and unclogs pores.
- Microdermabrasion: A gentle exfoliating treatment that removes dead skin cells and promotes collagen production.
- Blue Light Therapy: A pain-free treatment that targets acne-causing bacteria.
- Laser Treatment: A precise treatment that reduces inflammation and prevents scarring.
Chemical Peels: A Non-Invasive Solution
Chemical peels are a popular acne treatment option that uses a solution to exfoliate the skin and unclog pores. This non-invasive treatment is perfect for those who want to avoid harsh chemicals or surgery.
Microdermabrasion: Exfoliate Your Way to Clear Skin
Microdermabrasion is a gentle exfoliating treatment that removes dead skin cells and promotes collagen production. This treatment is ideal for those with mild to moderate acne.
Blue Light Therapy: A Pain-Free Treatment
Blue light therapy is a pain-free treatment that targets acne-causing bacteria. This non-invasive treatment is perfect for those who want to avoid harsh chemicals or surgery.
Laser Treatment for Acne Scars and Hyper-Pigmentation
Laser treatment is a precise treatment that reduces inflammation and prevents scarring. This treatment is ideal for those with severe acne or acne scars.
Home Care Tips for Maintaining Clear Skin
While professional treatment is essential, home care plays a crucial role in maintaining clear skin. Here are some tips to keep your skin healthy:
- Wash your face twice a day: Use a gentle cleanser to remove dirt and impurities.
- Exfoliate once a week: Use a gentle exfoliator to remove dead skin cells.
- Use sunscreen: Protect your skin from UV rays that can cause acne.
Common Acne Myths Busted
There are many myths surrounding acne, but what’s fact and what’s fiction? Here are some common acne myths busted:
- Myth: Acne is caused by poor hygiene.
- Reality: Acne is caused by a combination of factors, including hormonal fluctuations, genetics, and stress.
The Role of Diet in Acne Treatment
Diet plays a crucial role in acne treatment. Here are some foods that can help reduce acne:
- Leafy greens: Rich in antioxidants and fiber, leafy greens can help reduce inflammation.
- Berries: Rich in antioxidants and vitamins, berries can help reduce inflammation.
Stress and Acne: What’s the Connection?
Stress can trigger hormonal fluctuations, which can lead to acne. Here are some stress-reducing techniques that can help:
- Meditation: Reduces stress and anxiety.
- Yoga: Reduces stress and improves flexibility.
How to Choose the Right Acne Treatment for Your Skin
Choosing the right acne treatment in Punjabi Bagh can be overwhelming, but here are some tips to help:
- Consult a dermatologist: A dermatologist in Punjabi Bagh can help you identify the underlying causes of your acne.
- Consider your skin type: Different skin types require different treatments.
Conclusion: Say Goodbye to Acne with Dr. Vijay Singhal
Acne can be frustrating, but with the right treatment, you can say goodbye to acne for good. Dr. Vijay Singhal at Zenith Skin & Dental Clinic offers expert acne treatment in Punjabi Bagh that addresses the root cause of your skin concerns. Book your appointment today and get ready to glow!
Frequently Asked Questions (FAQs)
Q: What is acne and why does it happen?
A: Acne is a common skin condition that occurs when the pores on your skin become clogged with dead skin cells, oil, and bacteria. The exact cause of acne is still unknown, but factors like hormonal fluctuations, genetics, and stress can contribute to its development.
Q: What are the different types of acne?
A: There are several types of acne, including comedonal acne (whiteheads and blackheads), inflammatory acne (papules, pustules, and cysts), and more.
Q: Why is professional acne treatment important?
A: Professional acne treatment is essential for long-term results. A dermatologist can help you identify the underlying causes of your acne and create a personalized treatment plan.
Q: What are the acne treatment options available at Zenith Skin & Dental Clinic?
A: Zenith Skin & Dental Clinic offers a range of acne treatment options, including chemical peels, microdermabrasion, blue light therapy, and laser treatment.
Q: How can I maintain clear skin at home?
A: To maintain clear skin at home, wash your face twice a day, exfoliate once a week, and use sunscreen to protect your skin from UV rays.